The BMI (Body Mass Index) is used internationally, both by healthcare professionals and individuals. It is used to evaluate someone’s corpulence based on a 7-degree scale. The formula to calculate it is simple:
BMI = weight(kilograms) / height²(meters)
Here are the different levels of interpretation according to the World Health Organization:
- Below 16.5: malnutrition
- Between 16.5 and 18.5: underweight
- Between 18.5 and 25: normal corpulence
- Between 25 and 30: overweight
- Between 30 and 35: moderate obesity (class 1)
- Between 35 and 40: severe obesity (class 2)
- Below 40: extreme obesity (class 3)
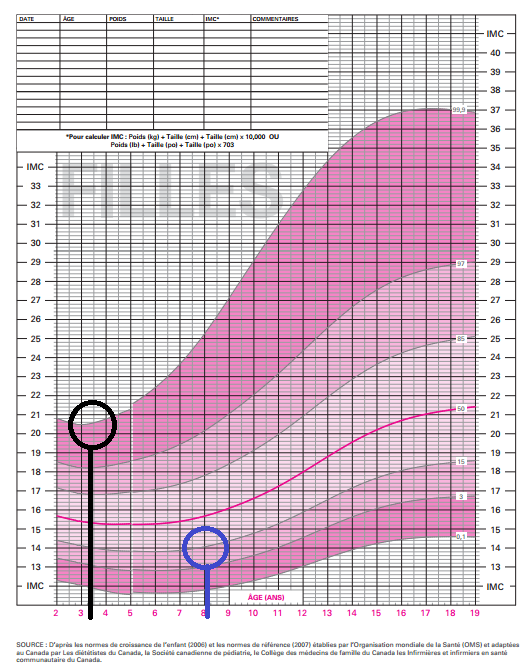
These results above only apply to adults or people above the age of 20. For children and teenagers, whose fat and muscle mass are still undergoing changes, BMI is calculated differently. Doctors and health professionals refer to the curve recorded in the person’s health book) to analyse the evolution. The lowest point on this curve is called the “adiposity rebound”, which usually occurs around the age of 6, and is normally followed by a progression. When the rebound occurs at an earlier age, this can lead to higher risk of obesity.
How is BMI an indicator of good or bad health?
The BMI gives an indication of a medically ideal body size which should ideally be around 22. BMI is different to fitness weight, which is the weight level where individuals feel comfortable with , both physically and psychologically. These two ideal weights are complementary.
Health professionals use BMI because it provides a global view of one’s health. Indeed, it allows to anticipate the risks of pathologies or chronic diseases such as diabetes, hypertension, cholesterol, stroke risks, joint problems and many other pathologies. In addition, people with high BMI have a higher risk of infertility, cancer and chronic diseases. High BMI’s can influence life expectancy reduction to about 4 years, as well as for people with too low BMI’s. BMI index is also used by statisticians assessing the level of obesity of a population in order to launch relevant and properly targeted prevention campaigns.
An index regularly questioned
Although this method of calculation is widely used, it is not flawless and may even prove inaccurate in some cases. The reason being that it does not take into consideration gender, age, ethnicity, sporting and physical habits, etc. It also does not take into account the relationship between muscle mass and fat mass, only the excess of the latter being harmful to health. The BMI is therefore useful as a reference index, but its calculation remains approximate to determine health risks.
Other approaches such as measuring of waist (which is based on the waist/hip ratio) could be more appropriate, as it is directly correlated with the risk of obesity (type 2 diabetes and cardiovascular disease). So-called abdominal obesity is indeed the most dangerous for health. It is characterised by a waist circumference of more than 94 cm for men and 80 cm for women.
BVI, or Body Volume Index, can also be a relevant alternative to BMI, as it evaluates abdominal volume based on the distribution of fat mass and lean mass. Although its calculation is much more complex, making it impossible to do it yourself at home, it is nonetheless an excellent prevention tool against obesity.
For several years now, researchers and scientists have been working on the subject and, thanks to new technologies such as 3D scanning, it is now possible to know your BVI using a mobile application. All that is required is taking a front and profile picture, which takes just over 30 seconds. For the moment this application is only accessible to experts and healthcare professionals because it is not yet optimized for general public use. However, it is already a major step forward in the assessment of medical risks among worldwide populations.
BMI in health insurance
For any insurer specializing in health coverage, BMI is an indicator of the risk of cardiovascular accidents and increases in other risk factors. An individual’s BMI will therefore be considered in the calculation of the insurance premium, along with the assessment of his or her general condition and preexisting conditions. This assessment only applies when the insured completes a medical questionnaire. In the case of the moratorium, the individual’s weight and height will not be reported; all risks related to weight issues (and preexisting conditions) will therefore be automatically excluded from the insurance cover.
So what are the advantages and disadvantages of BMI?
Although the use of BMI alone is not sufficient for the reasons mentioned above, the well-known body mass index does have its advantages:
- The calculation of BMI is very simple and allows a quick assessment of weight-related health risks
- It is an international standard approved by the WHO and used by all health professionals
What are the flaws of BMI? It has its limitations and drawbacks, which you should take into account for a more accurate interpretation of your health:
- It does not give any indication of the fat/muscle mass ratio, age, sex or morphology of the person. It gives clues to the patient’s state of health, but only a doctor can make a full diagnosis.
- It cannot be used alone in public health studies, as it tends to become obsolete. It must therefore be combined with other measurement tools.


